For a long time, people suffering from persistent symptoms following Lyme disease treatment often encountered doubt from both medical professionals and society in general. These people experienced ongoing tiredness, aching joints, cognitive challenges, and neurological problems, despite finishing typical antibiotic treatments. Although these symptoms were genuine for sufferers, the idea of “chronic Lyme disease” continued to be debated in medical circles. However, today there is a clear change in the way this condition is being recognized and managed by healthcare providers.
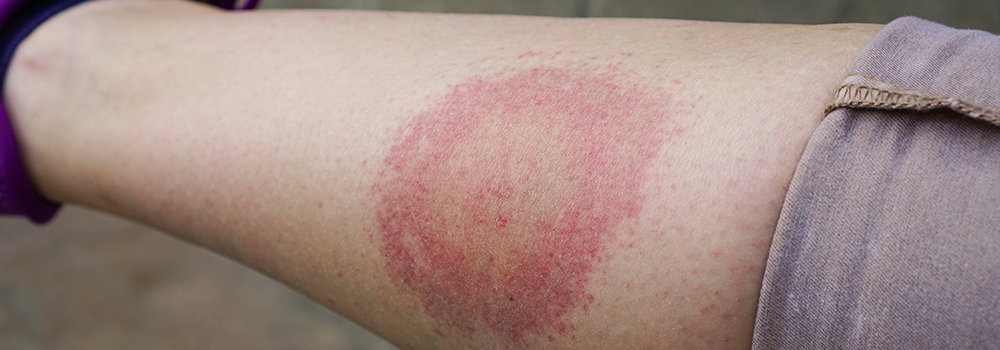
Lyme disease, resulting from the bacterium Borrelia burgdorferi and spread by the bite of infected blacklegged ticks, stands as the most prevalent vector-borne illness in the United States. Initial signs often encompass fever, tiredness, headache, and a distinctive skin rash. If diagnosed promptly, the condition is usually manageable with antibiotics. Nonetheless, a significant number of individuals experience symptoms that linger even after therapy. These ongoing symptoms have sparked years of discussion regarding what is currently referred to as “Post-Treatment Lyme Disease Syndrome” (PTLDS).
The term PTLDS is increasingly favored among clinicians as it distances the diagnosis from controversial connotations associated with “chronic Lyme disease” while acknowledging that a subset of patients do continue to suffer long-term effects. Recent years have seen a growing number of doctors who are open to the idea that these post-treatment complications warrant medical validation and active management, rather than dismissal or psychosomatic attribution.
A contributing factor to the changing viewpoint is the gathering of patient-reported information and medical research indicating that a more intricate process occurs in the body after infection. Scientists are investigating multiple hypotheses, such as immune system imbalance, residual bacterial particles causing inflammation, or even the possible influence of additional infections carried by ticks. Although no single theory has achieved widespread agreement yet, the growing body of evidence has paved the way for more research.
Otra razón detrás de este cambio de actitud es la creciente visibilidad de la enfermedad de Lyme. El cambio climático ha ampliado el hábitat de las garrapatas, lo que ha provocado un aumento de casos en áreas antes vistas como de bajo riesgo. Más personas, incluyendo médicos y funcionarios de salud pública, ahora conocen a alguien afectado por problemas crónicos relacionados con Lyme, otorgándole a la enfermedad una mayor legitimidad e importancia.
The conventional method for addressing Lyme disease typically involves administering antibiotics for several weeks. This approach proves successful for numerous individuals, though not for every patient. Those who continue to experience symptoms often feel frustrated when test results indicate no ongoing infection, and physicians find it challenging to provide effective solutions. This situation has contributed to the emergence of a medical gray area, where patients switch between specialists or resort to alternative treatments beyond conventional medicine. Regrettably, the absence of uniform medical direction has occasionally exposed patients to unvalidated therapies or potential medical exploitation.
Recognizing these gaps, some medical institutions are beginning to launch dedicated centers focused on tick-borne illnesses and persistent Lyme symptoms. These programs aim to offer more comprehensive care, incorporating neurology, immunology, and rehabilitation into treatment plans. They also emphasize listening to patient experiences and validating their symptoms, even when standard diagnostics fall short.
Still, not all corners of the medical world have embraced the shift. There remains skepticism about whether ongoing symptoms are directly caused by Lyme disease or result from other conditions or psychosomatic responses. Critics of the “chronic Lyme” label argue that misdiagnosis could lead patients down a path of unnecessary treatment or missed detection of other health issues. However, proponents of broader recognition argue that dismissing persistent symptoms leaves patients unsupported, often worsening their condition due to stress, delayed care, or emotional strain.
Insurance coverage is another barrier. Many health plans limit coverage to short-term antibiotic regimens and do not reimburse for extended treatments or multidisciplinary care, citing insufficient evidence. As the conversation around PTLDS grows and new research efforts receive funding, it’s possible that future clinical guidelines may evolve to better reflect the needs of these patients and improve care access.
Central to the situation is an increasing realization that complicated conditions such as post-treatment Lyme disease do not always align neatly with conventional diagnostic categories. Similar to how the medical community has gradually grasped the persistent impacts of COVID-19, there is a growing acknowledgment that infectious illnesses can occasionally result in enduring health issues that persist far beyond the end of the acute phase of the infection.
At the same time, individuals with lingering symptoms following Lyme therapy persist in searching for explanations, frequently navigating through a challenging path of advocacy, experimentation, and disjointed healthcare. The continual advancement in medical comprehension brings a ray of optimism—not just for acknowledgment, but also for more efficacious treatments, amplified research funding, and an increased focus on comprehensive patient care.
As Lyme disease awareness continues to grow and science digs deeper into its long-term impact, the line between doubt and diagnosis may finally begin to blur. This shift marks a critical step toward building a more compassionate, informed, and scientifically grounded approach to treating individuals whose suffering has long gone unrecognized.